Conditions
Cervicogenic Headache
“In terms of basic sciences, cervicogenic headache is the best understood of all the common headaches. The mechanisms are known, and this headache has been induced experimentally in healthy volunteers.“
Nikolai Bogduk and Jayantilal Govind
Cervicogenic headache literally means a headache ’caused by (genic) the neck (cervico)’. This seemingly should make it one of the simplest forms of headache to diagnose, yet it has a checkered and controversial existence.
Despite the association of neck pain and headache dating back to 400BC cervicogenic headache was first scientifically described in 1983. The purpose was to define a type of headache that was caused by neck complaints, but the challenge was that it had to be ‘clearly distinct’ from existing headache types – namely migraine and ‘muscle contraction’ (now known as tension-type) headache. This was, and continues to be a challenge due to the fact that:
- Symptoms associated with cervicogenic headache can include severe pain, nausea, vomiting, sensitivity to light and sound, dizziness. In other words it can be almost impossible to distinguish cervicogenic headache from migraine based on symptoms alone.
- The vast majority of headache sufferers report neck pain before, during and/or after and attack.
- The majority of migraine and tension-type headache sufferers can have their ‘familiar pain’ reproduced with manual examination (pressure) on the upper cervical spine but this is often ignored or poorly understood as the discipline most commonly assessing sufferers (Neurology) is not well trained in examination of the spine.
As Neurologist Werner Becker describes:
Neurologists are the specialist to whom headache patients are referred to most often, and neurologists are often not expert in the examination of the neck.
What we have then is a description of a particular type of headache very obviously caused by a problem in the neck, and very clearly not a migraine or tension-type headache. As we will see below, up to 80% of migraine and tension-type headache have the neck as a source of symptoms. In many of these cases the neck itself is not particularly symptomatic.
Diagnosis & Symptoms
To diagnose a cervicogenic headache as distinct from migraine or tension-type headache the Cervicogenic Headache International Study Group (CHISG) describe the following criteria:
- Unilateral (one sided) or unilaterally dominant – This does allow for milder symptoms to be felt on the other side (unevenly bilateral) but not for evenly bilateral headache.
- Side-locked (does not swap sides – sideshift).
- Associated with neck, shoulder or arm pain on the same side (ipsilateral).
- Pain begins in the neck and headache is aggravated by neck movement or neck postures. 1 2
Currently the International Headache Society (IHS) classification for Cervicogenic Headache is:
Headache caused by a disorder of the cervical spine and its component bony, disc and/or soft tissue elements, usually but not invariably accompanied by neck pain.
Diagnostic Criteria:
A. Any headache fulfilling criterion C
B. Clinical and/or imaging evidence of a disorder or lesion within the cervical spine or soft tissues of the neck, known to be able to cause headache
C. Evidence of causation demonstrated by at least two of the following:
- headache has developed in temporal relation to the onset of the cervical disorder or appearance of the lesion
- headache has significantly improved or resolved in parallel with improvement in or resolution of the cervical disorder or lesion
- cervical range of motion is reduced and headache is made significantly worse by provocative manoeuvres
- headache is abolished following diagnostic blockade of a cervical structure or its nerve supply
D. Not better accounted for by another ICHD-3 diagnosis
Among the notes includes the following:
Features that tend to distinguish Cervicogenic headache from migraine and tension type headache include side-locked pain, provocation of typical headache by digital pressure on neck muscles and by head movement, and posterior-to-anterior radiation of pain. However, while these may be features of Cervicogenic headache they are not unique to it and they do not necessarily define causal relationships.
Migrainous features such as nausea, vomiting and photo/phonophobia may be present with cervicogenic headache, although to a generally lesser degree than in migraine.
With up to 70% of migraineurs and even more tension-type headache sufferers having neck pain at some stage during an attack its easy to see how hard it is to distinguish between groups.
Epidemiology
0%
of all headaches.0%
diagnosed as 'cervicogenic headache'.0%
remain undiagnosedReports on the prevalence of cervicogenic headache vary wildly, according to how the researchers chose to diagnose it, whether they used self reporting or direct examination, and which criteria (CHISG or IHS).
The CHISG criteria which describes a symptomatic approach the estimates are quite low ranging from 0.1%, 2.5% to 4.1% as the upper limit.
However a key study from 1995 using what became the IHS criteria – diagnostic blocks of joints in the upper cervical spine, then up to 80% of headaches were able to be diagnosed as cervicogenic, despite none of them having that diagnosis to begin with.
Equally as informative are studies of people with chronic post whiplash symptoms. One study found injecting the C2/3 zygapophysial joint abolished headache in 53% of headache sufferers, whilst another study described 112 patients who had chronic post traumatic (whiplash) headache with no significant past history of headache. The amazing thing was they presented with a wide variety of headache types; 37% had tension-type headache, 27% migraine, 18% cervicogenic headache and 18% had headaches that were of mixed type or didn’t fit a classification.
Clearly if whiplash can induce tension-type headache and migraine the neck is involved, and seemingly the C2/3 segment seems implicated in a majority of cases. Importantly, these are generally not diagnosed as cervicogenic headache. In other words from a symptomatic and functional point of view the neck is not obviously dysfunctional, yet the anaesthetic blockades are proving the neck is the driving force in up to 80% of presentations.
Common Treatments
Cervicogenic headache is the most common form of headache presenting to local therapy clinics (physiotherapy, chiropractor, osteopathy, massage, acupuncture etc). Many one off and simple cases will do well in these clinics with a short bout of treatment.
Cervicogenic Headache Treatment – First episode
The first time you present with neck pain, restriction of neck movement and an accompanying headache – don’t call us. Find a physiotherapy clinic (or other familiar manual therapist) near where you live and book in to see someone. The likelihood is with some treatment to re-establish movement, your symptoms will subside and you may never have an issue again.
Recurrent Cervicogenic Headache Treatment
The regular recurrence of neck pain, restriction of movement and headache should not be treated the same way as above – but it so often is. Someone pushes on your neck to ‘loosen everything up’ but the cause of the problem hasn’t been rectified, so you are just a matter of time before it happens again.
- Recurrent bouts of cervicogenic headache are often over-treated.
- An alarm should ring for you if:
- Your treatment is the same for each bout – you will get the same (recurrent) result)
- Your therapist is unable to explain why you are still getting symptoms and what it is they will do differently to target the underlying problems.
- Often you will need to refer yourself to a specialised treatment centre like our for lasting results.
There are three ways to approach treating cervicogenic headache:
- Press and guess
- Treat everything
- Target the most sensitive structures first
Press and guess:
This can work well for those initial episodes. Find the sore bit and push. Often isolated episodes are caused by a joint in the spine becoming painful. By stretching it and loosening up the muscle spasm around it the source of the local pain (and often referred pain) will go. Unfortunately, the most common response to recurrent episodes is to do the same thing over and over, getting short term relief with recurrent bouts of the same problem, or even worse, aggravation of symptoms with techniques that are too aggressive.
Treat Everything
Hopefully you have a therapist who will at least look at muscle strength, muscle length, posture and maybe even balance and joint position error. The problem is that people without pain or symptoms will test positive on some of these tests. So which things are important? This will lead to a treatment program that can last months while you strengthen your deep flexors, do pilates for your thoracic strength and posture, stretch your shortened neck muscles and strengthen your middle and lower trapezius. Hopefully……one of these might help! It’s a long process, and somewhat of a ‘stretch and strengthen and guess’ approach – though one that has higher chance of success than press and guess.
Treat the most sensitive structures first
There is a dysfunction affecting the upper cervical spine present in almost everyone (due to our development – a big heavy head and a weak spine) that if it becomes sensitive can not only cause cervicogenic headache, but tension-type headache, migraine, vestibular migraine and cyclic vomiting syndrome.
This dysfunction doesn’t always cause neck pain, which is why the prevalence of cervicogenic headache is low. Identified by Dean Watson, and treated using his Watson Headache® Approach targeting the a painful disturbance at the level of C2/C3. This causes a protective spasm in a small muscle in the top of the neck. The stress this small muscle creates feeds directly into pain centres in the brainstem known to be overactive in all forms of headache.
The great thing is we can treat successfully within a matter of weeks, not months. It is targeted, rapid, and takes away the greatest source of noise. Very few people will then need to go on a complete the ‘stretch and strengthen and guess’ approach highlighting the fact that some dysfunction is ‘normal’.
Causes
The trigeminal nerves provide sensory feedback from the head and face.
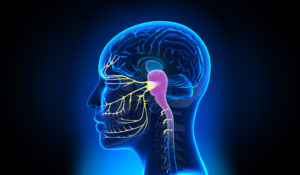
They enter the brainstem and terminate at the same place as the upper three cervical nerves. At this point there is significant convergence between the two systems, with up to 40% overlap between cervical and trigeminal nerves.
According to the world renowned Australian anatomist, Nicolai Bogduk the cause of headaches:
can be summarised as any primary cause that activates the trigeminal nucleus. Given the appropriate stimulus and given the appropriate convergent connections in the central nervous system, any structure innervated by the C1, C2, C3 cervical nerves and the cranial nerves V (trigeminal), IX (glossopharyngeal) and X (vagus), is capable of causing headache. 3
From the neck these structures include:
- Nerves and nerve root ganglia
- Uncovertebral joints
- Intervertebral disks
- Facet joints
- Bone (including periosteum)
- Muscles
- Ligaments
- Blood vessels
- Dura around brainstem and posterior fossa (cerebellum)
Problems arising with any of these structures is signalled back via the upper three cervical nerves into the brainstem – into the same part of the brainstem that houses the trigeminal nerve receiving input from the head and face as well as the throat and ear from cranial nerves IX and X.
Convergence of these inputs allows signals from neck structures to be confused with signals from the head and face which forms the essence of referred pain – in this case a headache.
Differential Diagnosis
Due to the highly variable presentation of cervicogenic headache differentiating it from migraine and tension type headache is very challenging. Whilst the classification makes them look like distinctly different, which they need to be for research, in reality there’s significant overlap – many start with TTH and might stay that way or progress and become migraine. If your cervicogenic headache is ‘unilateral on both sides’ there is nothing that will distinguish it from tension type headache.
The only way to know is to test the upper cervical spine for sources of pain. Can we reproduce familiar head-pain with palpation of structures in the upper cervical spine, and does treating these structures result in a significant and lasting change in headache presentation.
Dissecting aneurysm – vertebral and internal carotid arteries : Important to exclude with acute onset headache with a severe neck pain that will be described like a tearing/fearful pain unlike any neck pain they have experienced before. Inappropriate treatment (spinal manipulation) of these patients can be catastrophic, whereas early diagnosis and detection can avert development of cerebrovascular symptoms.
Posterior fossa lesions: this incorporates things like tumours, meningiomas, astrocytomas, medulloblastomas etc. Space occupying lesions of the posterior fossa will compress the dura which in the posterior fossa is innervated by the upper cervical nerves. Symptoms occur very early and can include drowsiness, headache, imbalance, ataxia (due to cerebellar involvement), nausea and neck pain.
Meningitis of the upper cervical spine: the onset of a sudden high fever with a stiff neck and severe headache that is different to any headache they have experienced before, nausea and or vomiting, seizures, sleepiness, confusion.
Herpes Zoster: can produce occipital pain in the region during the prodrome, however it is readily distinguished from cervicogenic headache with the eruption of vesicles as the condition progresses.
Neck-tongue syndrome: numbness of the tongue accompanied by ipsilateral (same sided) occipital pain may occur with subluxation of the lateral C1/2 (atlanto-axial) joint. This can occur with rapid turning of the head (e.g. whiplash, manipulation)
C2 Neuralgia: sharp lancinating pains in the occipital region accompanied by tearing (lacrimation) and engorgement of the ciliary arteries (ciliary injection).
Learn More
Learn more about our unique treatment, and what to expect during out consutations
